Mesothelioma prevention with inhaled vaccine?
By Kathy Cooke. 21st April 2021
Most vaccines are given as an injection into the muscle tissue, however many viruses infect people via mucosal surfaces such as the lining of the respiratory tract.
Mucosal surfaces provide an barrier between people and the outside environment and play an important role in protection against infection.
Examples include gastric, intestinal, nasal and the tongue. They help to keep the surrounding tissue moist and play a role in absorbing nutrients.
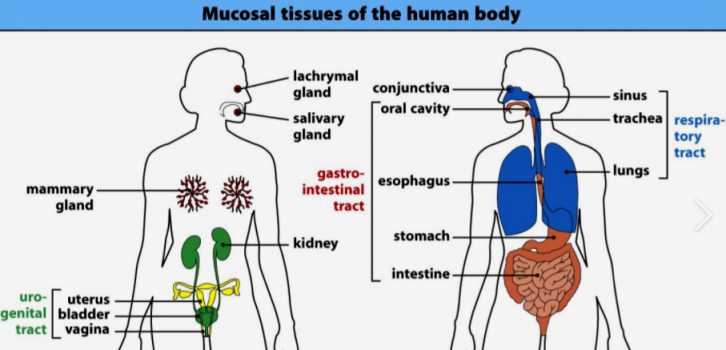
Lung infections often start on mucosal membranes, so researchers at MIT have recently developed a vaccine that binds to a protein in the mucus. They hope that the vaccine, when inhaled may trigger an immune response against infections and even cancer in the lungs. This could be important for people at risk of developing pleural mesothelioma.
The researchers at MIT (Massachusetts Institute of Technology) have now developed a vaccine that can create a multitude of T-cells that are ready and waiting at those surfaces, offering a rapid response to viruses. T-cells are white blood cells that originate in bone marrow and mature in the thymus (a gland in the chest between the lungs). In the thymus, T cells multiply and differentiate into helper, regulatory, or cytotoxic T cells or become memory T-cells. If T-cells recognizes cancer cells as the enemy, they can kill them before the cells turns into a tumour.
The researchers at MIT showed that it was possible to create a strong memory T-cell response in the lungs of mice by giving them a vaccine modified to bind to a protein naturally present in mucus. This can help ferry the vaccine across mucosal barriers, such as the lining of the lungs.
Senior scientist, Professor Darrell Irvine said of the study:
“ In this paper, we specifically focused on T cell responses that would be useful against viruses or cancer, and our idea was to use this protein, albumin, as sort of a Trojan horse to get the vaccine across the mucosal barrier ”
Inhaled vaccines can be used to treat asbestos lung cancer and pleural mesothelioma from metastasizing to the lungs or even prevent these cancers from developing in the first place.
Irvine continues . . .
“ In some cases, vaccines given in muscle can elicit immunity at mucosal surfaces, but there is a general principle that if you vaccinate through the mucosal surface, you tend to elicit a stronger protection at that site . . . Unfortunately, we don’t have great technologies yet for mounting immune responses that specifically protect those mucosal surfaces. ”
Delivering peptide vaccine to the back of the throat
Currently there is a nasal vaccine for the flu and an oral vaccine for Typhoid, however these are basically weakened forms of the germ that causes a diseases. The MIT researchers wanted to create something different: a peptide vaccine, which is safer and easier to manufacture, but more difficult to get across mucosal barriers.
In an attempt to make it easier to deliver the vaccine to the lungs, the MIT researchers attaching peptide vaccines to albumin proteins. Albumin is a made by the liver and helps to keep fluid in your bloodstream so it doesn't leak into other tissues. It is also carries various substances throughout your body, including hormones, vitamins, and enzymes. It can also easily pass through the tissue surrounding the lungs. The Albumin helped to build up the vaccine in the lymph nodes, where they could activate a strong T-cell response.
The researchers delivered vaccine intratracheally - to the back of the throat - to simulates inhalation exposure. They that this type of delivery generated a 25-fold increase in memory T-cells in the mouse lungs, compared with injecting the vaccine into a muscles as close as possible to the lungs. They also showed that when mice were exposed to the vaccinia virus months later, the intramuscular vaccine offered no protection, while all of the animals that received the vaccine intratracheally were protected.
Targeting tumours including mesothelioma and asbestos lung cancer
The researchers also tested a mucosal vaccine against cancer using a peptide found on melanoma cells to immunise mice. After the mice were vaccinated, they were exposed to melanoma cells and the T-cells in the lungs were able to destroy them. The scientists also showed that the vaccine could help to shrink existing lung tumours, again this is good news for victims of mesothelioma and asbestos lung cancer.
This kind of local response could make it possible to develop vaccines that would prevent tumors from forming in specific organs, by targeting antigens commonly found on tumour cells.
Professor Irvine concludes:
“ In both the virus and the tumor experiments, we’re leveraging this idea that, as other people have shown, these memory T cells set up shop in the lungs and are waiting right there at the barrier. As soon as a tumor cell shows up, or as soon as a virus infects the target cell, the T cells can immediately clear it. ”
If you have any questions, or would like some advice on whether you could claim compensation for an asbestos disease such as mesothelioma, please call on the number below and ask for Kathy or Warren

Sources
1. MIT. March 19, 2021. Delivering vaccines directly to the lungs can boost immune responses to respiratory infections or lung cancer
https://news.mit.edu/2021/vaccination-inhalation-0319
Author
Kathy Cooke MA. BSc
Cancer consultant and advisor
Kathy has worked in the cancer field for over 30 years. She was course leader for the MSc in Radiotherapy and Oncology at University of Hertfordshire. Then pre-treatment radiotherapy manager at the Cromwell Hospital in London and Partnership Quality Lead for Macmillan Cancer Support.. Read more >